Letter to editor
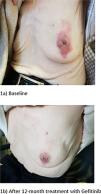
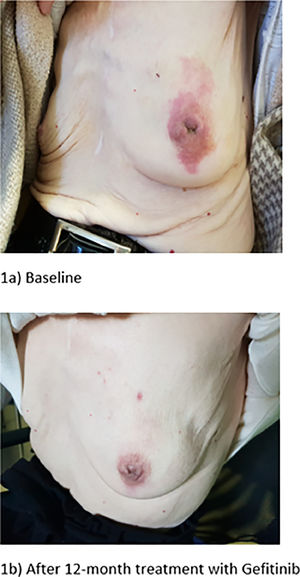
Breast metastases from extramammary tumors are rare, with a reported frequency of 0.2%-1.3%.1 Tumors known to metastasize to the breast have very diverse origins, including leukemias, lymphomas, lung cancer, among others.2,3 In this context, histology, and immunohistochemistry (IHC) characterization is essential for correct diagnosis and therapeutic guidance. The differential diagnosis with primary breast cancer may be challenging, considering it is the leading cause of cancer in women.4 Although luminal cancers are the most frequent, triple-negative breast cancer (TNBC) should be considered a plausible hypothesis, even in older women.5 These tumors are usually poorly differentiated, making a routine diagnosis even more challenging. Lung carcinoma is the second most common cancer among females6 and the most common sites of metastasis are the liver, adrenal gland, bone, and brain,7 while metastasis to the breast accounts only 0.4–1.3%.5 Lung cancer diagnosis has markedly evolved in the last decades, with new molecular and genetic biomarkers being routinely used. Epidermal growth factor receptor (EGFR) mutations occur in 10%–20% of Caucasian patients with lung adenocarcinomas.8 The advent of targeted therapies has modified the advanced lung adenocarcinoma treatment paradigm, with unprecedented outcomes and tolerability. We report a case of an elderly woman with breast metastasis of lung adenocarcinoma and previous history of breast carcinoma. To the best of our knowledge, until 2022 fewer than thirty such cases have been described.2 An 81-year-old non-smoker woman, with a history of breast carcinoma treated with tumorectomy 40 years ago, arterial hypertension, and dyslipidaemia, presented to the emergency department in May 2018 with dyspnoea of sudden onset with the evolution of 2 hours, aggravated by exertion, accompanied by asthenia and anorexia with 2 weeks of evolution. She had a mammogram revealing an irregular mass, in the transition of the upper quadrants of the left breast left, suspicious of malignancy (Breast imaging-reporting and data system (BiRADS) 5 - highly suggestive of malignancy). The referred lesion was evident on physical examination, presenting 4 cm, with nipple inversion and surrounding erythema (Fig. 1a). Chest X-ray revealed a large volume left pleural effusion, so diagnostic and evacuative thoracentesis was performed. Pleural fluid analysis was consistent with an exudate and a sample for cytology was collected. After symptomatic improvement, the patient was discharged and referred to the Oncology department. While waiting for the breast biopsy result, pleural fluid cytology revealed the presence of lung adenocarcinoma cells (thyroid transcription factor-1 (TTF-1) +, programmed death-ligand 1 (PD-L1) 0%, and EGFRexon21 mutation) and a thoracic computerized tomography scan showed a left lung mass and radiologic findings suggesting lymphangitic carcinomatosis. Considering the patient's age and comorbidities, it was decided to start palliative treatment with gefitinib (anti-EGFR Tyrosine Kinase Inhibitor (TKI)). With a strong clinical suspicion of breast cancer, the biopsy with an aggressive morphology and a negative immunohistochemical profile (lack of expression of the steroid hormone receptors (oestrogen and progesterone), and the human epidermal growth factor receptor-2 (HER-2)), the diagnosis of TNBC was assumed. Subsequently, integrating the whole clinical history, additional immunochemical with TTF1 was performed, which showed diffuse staining, favouring the diagnosis of metastasis of lung adenocarcinoma rather than primary breast cancer. Based on this information, the patient maintained gefitinib, presenting a rapid and objective response with partial regression of the pulmonary tumor, pleural effusion, and breast metastasis. The patient had good tolerance to gefitinib, with no remarkable side effects. Twelve months later, the patient was alive, with no pleural effusion and partial response of lung and breast lesions. (Fig. 1b). After eighteen months the patient had mesenteric ischemia, apparently unrelated to the oncologic treatment. IHC and molecular markers have a crucial role in oncology, contributing to more accurate diagnosis, tailored treatments, and improved prognosis. Although autopsy series have demonstrated that lung cancer can spread to almost every organ,5 the breast is a rare site.7 Breast metastasis from lung cancer represents less than 0.1%1 of breast malignant lesions and can mimic TNBC, requiring careful clinical and pathological differential diagnosis.9 Distinguishing breast metastasis from primary breast cancer based solely on clinic-radiological findings may be hard, impairing treatment decisions and patients’ outcomes.10 Breast metastasis of lung adenocarcinoma is an unexpected diagnosis in an elderly woman with a history of breast carcinoma and a new highly suspicious breast lesion. However, the detection of a pulmonary mass, with the described cytologic alterations, had broadened the diagnostic hypotheses. We must combine clinical suspicion with the existing diagnostic tools, with emphasis on multidisciplinary assessment, including pathology, reconciling the morphological, IHC, and molecular aspects, as well as the clinical presentation. Consideration of extramammary malignancy metastasis is important when evaluating breast lumps with other clinical features. Even with a high suspicion of primary neoplasia, we should routinely use other markers, such as GATA3, mammoglobin, and GCDFP15 to confirm the mammary origin of the neoplasia. The importance of a multidisciplinary tumor board discussion when treating frail and symptomatic geriatric patients, is also of utmost importance, especially in the era of precision medicine, where we have access to targeted therapies with a strong impact on prognosis and quality of life.