As recommended by the World Health Organization (WHO), optimal management of MDR-TB cases can be ensured by a multi-speciality consultation body known as ‘TB Consilium’. This body usually includes different medical specialities, competences and perspectives (e.g., clinical expertise both for adults and children; surgical, radiological and public health expertise; psychological background and nursing experience, among others), thus lowering the risk of making mistakes – or managing the patients inappropriately, in order to improve their clinical outcomes.
At present, several high MDR-TB burden countries in the different WHO regions (and beyond) have introduced TB Consilium-like bodies at the national or subnational level to reach consensus on the best treatment approach for their patients affected by TB.
In addition, in countries/settings where a formal system of consultation does not exist, specialized staff from MDR-TB reference centres or international organizations usually spend a considerable amount of their working time responding to phone or e-mail clinical queries on how to manage M/XDR-TB cases.
The aim of this manuscript is to describe the different experiences with the TB Consilia both at the international level (European Respiratory Society – ERS/WHO TB Consilium) and in some of the countries where this experience operates successfully in Europe and beyond. The Consilium experiences are described around the following topics: (1) history, aims and focus; (2) management and funding; (3) technical functioning and structure; (4) results achieved.
In addition a comparative analysis of the TB Consilia in the different countries has been performed.
The multidrug-resistant tuberculosis (MDR-TB) and extensively drug-resistant TB (XDR-TB) epidemics (defined, respectively, as resistance to isoniazid and rifampicin, and to at least one fluoroquinolone and one injectable second-line anti-TB drug in addition to isoniazid and rifampicin) are both clinical and public health priorities.1–3
Over 480,000 cases of MDR-TB (and 100,000 of rifampicin-resistant TB)1 are challenging physicians and public health specialists around the world, as their treatment is long, expensive and difficult, due to frequent adverse events.2–10 Furthermore, the results are still largely suboptimal: the success rates are in fact low (in the order of 50% in MDR-TB patients, and of 20–30% in XDR-TB cases with drug resistance profiles beyond XDR).2,3,10
As recommended by the World Health Organization (WHO), optimal management of MDR-TB cases can be ensured by a multi-speciality consultation body known as a TB Consilium. This body usually includes different medical specialities, competences and perspectives (e.g., clinical expertise – both for adults and children; surgical, radiological and public health expertise; psychological background and nursing experience, among others), thus lowering the risk of making mistakes – or managing the patients inappropriately in order to improve their clinical outcomes.4–7
At present, several high MDR-TB burden countries in the different WHO regions have introduced TB Consilium-like bodies at a national or subnational level to reach consensus on the best treatment approach for their patients affected by TB.
It is in fact well known that selection of resistant strains of Mycobacterium tuberculosis is largely an artificial phenomenon11–13 and that the correct management of difficult-to-treat cases of TB is useful in limiting their development and spread.
Moreover, in countries/settings where a formal system of consultation does not exist, specialized staff from MDR-TB reference centres or international organizations usually spend a considerable amount of their working time responding to phone or e-mail clinical queries on how to manage M/XDR-TB cases.
The aim of this manuscript is to describe the different experiences with the TB Consilia both at the international level (European Respiratory Society – ERS/WHO TB Consilium) and in the some of the countries where this experience operates successfully in Europe and beyond (Belarus, Belgium, France, Mexico, Portugal and United Kingdom).
The Consilium experiences are described around the following topics: (1) history, aims and focus; (2) management and funding; (3) technical functioning and structure; (4) results achieved.
A comparative analysis of the Consilia in the different countries is summarized in Tables 1 and 2.
The ERS/WHO TB ConsiliumHistory, aims and focusThe ERS/WHO electronic TB Consilium platform was launched in September 2012, becoming the first global, free-access online mechanism allowing peer-to-peer clinical consultation for individual TB patients, storing data and allowing their analysis to evaluate whether existing prevention, diagnosis and treatment guidelines are properly followed.4,5
The ERS has demonstrated strong leadership and commitment to eliminating TB14,15 through different initiatives,16–18 including the TB Consilium.
The ERS-WHO electronic TB Consilium was launched during the 30th ERS Congress in Vienna, on 6th September 2012. On this occasion, the WHO Regional Office for Europe signed a Memorandum of Understanding with ERS to coordinate and co-manage this initiative.
Management and fundingThe ERS/WHO Consilium is managed technically by ERS through the ERS TB Collaborating Centre, in collaboration with WHO (Regional Office for Europe). ERS provides the necessary funding to support the activities and maintain the platform from core funds based on a detailed annual plan and a 3-year medium-term one.
Technical functioning and structureThe ERS/WHO TB Consilium has different functionalities.
The first and core function is clinical. It specifically provides scientifically sound and evidence-based advice globally to national Consilium bodies and individual clinicians on how to manage drug-resistant TB and other difficult-to-treat TB cases (including co-infection with HIV, paediatric cases and the challenging and adequate use of new drugs such as delamanid under compassionate use programme). Furthermore, by providing clinical guidance, the ERS/WHO TB Consilium contributes to preventing further development of drug resistance. Once sufficient data are stored, the TB Consilium will also allow monitoring and evaluating the quality of clinical practices in a given country or setting, in terms of prevention, diagnosis and treatment against established evidence-based guidelines.
The ERS-WHO TB Consilium operates rapidly: it answers the clinical questions posed within two working days. Following the clinician's upload, a case request (specifying the case details and the question(s) for the TB Consilium experts), the TB Consilium director receives the request in real time. The director then empowers a clinical coordinator, who identifies two experts through the Expert Roster (including >60 international TB experts from 22 countries). A call for experts (including TB clinicians, but also other professionals relevant for patient management, e.g. microbiologists, public health experts, psychologists, etc.) was launched by ERS and WHO (with the external support of ECDC – the European Centre for Disease Prevention and Control in Stockholm) preceded the activation of the service. The experts’ applications were evaluated by an international expert panel based on strict technical criteria, in agreement with Swiss Law.
The clinical coordinator then receives the experts’ opinions, moderates and consolidates them with precise instructions to be reported to the requesting physician.
The TB Consilium e-platform can be accessed free of cost at www.tbconsilium.org by any physician needing clinical support. The platform is multi-language (operating in English, Portuguese, Russian and Spanish).
The ERS-WHO TB Consilium platform has been presented to different countries, national TB programme managers and individual clinicians, and launched at the WHO TB Strategic Technical Advisory Group in Geneva, presented to the Childhood TB subgroup of the DOTS expansion group and regularly advertised by the ERS through its own publications [newsletter, European Respiratory Journal (ERJ), ERJ Open Research, European Respiratory Review, Breathe] and its website. Furthermore, the ERS-WHO TB Consilium has also been included in the curriculum of the WHO course for managers and consultants on how to apply the WHO's End TB Strategy, which is focused on the concept of TB elimination.14,15 It is organized twice a year in Cepina/Sondalo, Italy (www.publichealthcg.com), and replicated in different continents in different languages.
Results achievedThe TB Consilium interim results have been published elsewhere4,5 and presented in different international conferences and events.
The e-platform is evaluated at regular intervals.4–7 At present (Tables 1 and 2), 337 cases from 39 countries have been supported by this platform, including 24 cases in two different epidemics4,5: 230 with MDR-TB (135 being XDR), including 37 children and 61 TB cases requesting advice for a possible introduction of delamanid within the compassionate use programme (11 were non-eligible).
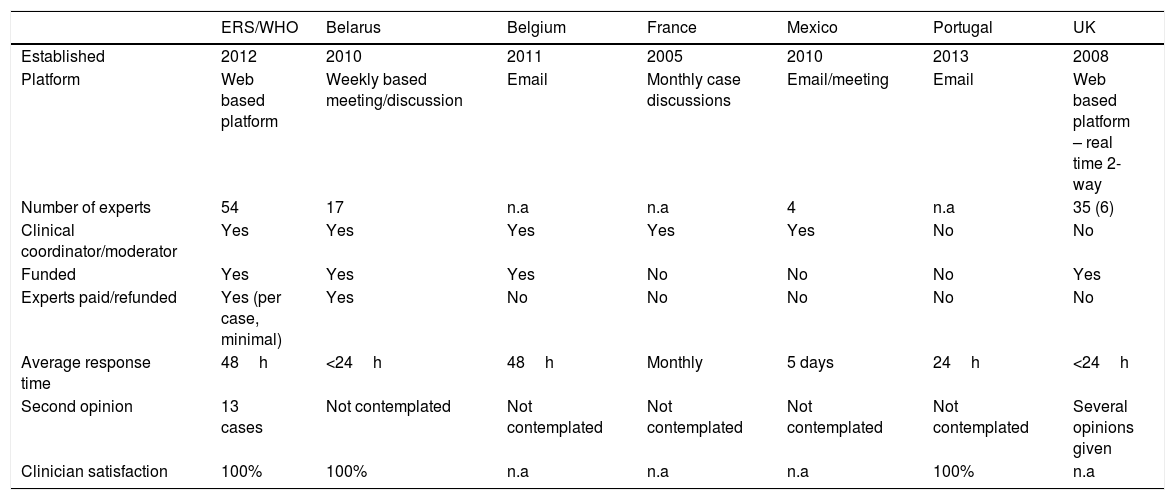
Summary of the main features of the international (ERS/WHO) and national TB Consilia compared.
| ERS/WHO | Belarus | Belgium | France | Mexico | Portugal | UK | |
|---|---|---|---|---|---|---|---|
| Established | 2012 | 2010 | 2011 | 2005 | 2010 | 2013 | 2008 |
| Platform | Web based platform | Weekly based meeting/discussion | Monthly case discussions | Email/meeting | Web based platform – real time 2-way | ||
| Number of experts | 54 | 17 | n.a | n.a | 4 | n.a | 35 (6) |
| Clinical coordinator/moderator | Yes | Yes | Yes | Yes | Yes | No | No |
| Funded | Yes | Yes | Yes | No | No | No | Yes |
| Experts paid/refunded | Yes (per case, minimal) | Yes | No | No | No | No | No |
| Average response time | 48h | <24h | 48h | Monthly | 5 days | 24h | <24h |
| Second opinion | 13 cases | Not contemplated | Not contemplated | Not contemplated | Not contemplated | Not contemplated | Several opinions given |
| Clinician satisfaction | 100% | 100% | n.a | n.a | n.a | 100% | n.a |
ERS: European Respiratory Society; WHO: World Health Organization; TB: tuberculosis; UK: United Kingdom; n.a: not available.
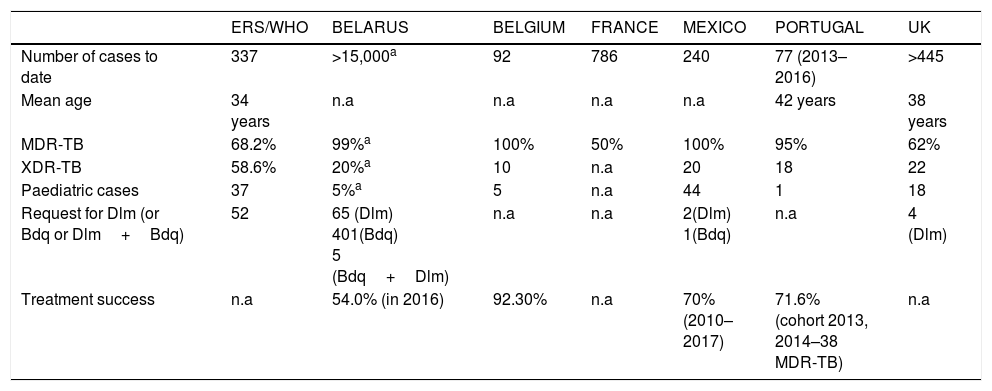
Summary of the main achievements of the international (ERS/WHO) and national TB Consilia compared (data expressed as percentages or absolute numbers as available).
| ERS/WHO | BELARUS | BELGIUM | FRANCE | MEXICO | PORTUGAL | UK | |
|---|---|---|---|---|---|---|---|
| Number of cases to date | 337 | >15,000a | 92 | 786 | 240 | 77 (2013–2016) | >445 |
| Mean age | 34 years | n.a | n.a | n.a | n.a | 42 years | 38 years |
| MDR-TB | 68.2% | 99%a | 100% | 50% | 100% | 95% | 62% |
| XDR-TB | 58.6% | 20%a | 10 | n.a | 20 | 18 | 22 |
| Paediatric cases | 37 | 5%a | 5 | n.a | 44 | 1 | 18 |
| Request for Dlm (or Bdq or Dlm+Bdq) | 52 | 65 (Dlm) 401(Bdq) 5 (Bdq+Dlm) | n.a | n.a | 2(Dlm) 1(Bdq) | n.a | 4 (Dlm) |
| Treatment success | n.a | 54.0% (in 2016) | 92.30% | n.a | 70% (2010–2017) | 71.6% (cohort 2013, 2014–38 MDR-TB) | n.a |
ERS: European Respiratory Society; WHO: World Health Organization; TB: tuberculosis; UK: United Kingdom; n.a: not available; MDR-TB: multidrug-resistant tuberculosis; XDR-TB: extensively drug-resistant tuberculosis; Dlm: Delamanid; Bdq: Bedaquiline.
The average time needed by the physician to upload the case's details into the electronic platform was estimated to be <30min by clients, with a mean value of 20min. All clinicians reported to be satisfied by the TB Consilium services.
A second function supporting the migrants’ transborder issues has recently completed pre-testing in collaboration with the WHO. The system allows clinicians managing a patient in a given country to liaise with the country where the patient is planning to migrate during TB treatment or where the patient is coming from so that data can be exchanged and continuum of care can be ensured, reducing loss to follow up.
In conclusion, the ERS/WHO TB Consilium represents an effective instrument to support the WHO End TB Strategy and TB elimination.14,15
The TB Consilium in BelarusHistory, aims and focusIn 2010 M/XDR-TB represented an emergency in Belarus, with a MDR-TB prevalence of 32.7% among new cases and 76.6% among previously treated cases and a prevalence of XDR-TB of 1.7% and 16.5% respectively.19 In TB/HIV co-infected patients, the prevalence of MDR-TB was consistently higher among both new (51.1%) and previously treated cases (100%). The MDR-TB treatment success rate was low and the mortality dramatically high. Routine monitoring in 2009–2010 showed that the WHO-recommended treatment regimens were not always correctly prescribed. In these conditions, the role of the Central MDR-TB Consilium was to expedite diagnosis and ensure that individual treatment regimens were correctly designed.20 In parallel with the improved skills of the specialists involved at the regional and peripheral level, the input required from the MDR-TB Central Consilium decreased. From 2013, based on recommendations of the Green Light Committee, the Regional Consilia started to work independently (reporting only difficult cases to the central level). While the Central TB Consilium session initially required three days, they are now managed in a single day.
In summary, the aim of the Central MDR-TB Consilium in Belarus is to improve MDR-TB treatment outcomes through a multidisciplinary approach to patient management. A priority was to train specialists in multidisciplinary Consilia, to enable them to work at a decentralized level in order to improve the quality of diagnosis and care and to reduce the time to initiation of effective MDR-TB treatment throughout the country.
Management and fundingConsilium activities were initially funded by the Global Fund. To ensure sustainability in regions and districts a Minister of Health's directive ensured coverage of transportation and per diem costs for Consilium officers to travel from the local to the Oblast (Regional) level, and when necessary to the national level for the Central Consilium. To maintain the experts’ skills, two courses per year were planned and budgeted by the National TB programme, while other training was done at the regional and penitentiary level.
Technical functioning and structureThe MDR-TB Consilium has the following functions: registering new MDR-TB cases, making decisions on treatment initiation, treatment regimens modifications and management of any other treatment issue including adverse events and indication for surgery, transferring of patients to palliative care, managing treatment loss to follow-up, performing cohort analysis and ensuring an uninterrupted supply of anti TB and other supportive medications. The MDR-TB Consilium in Belarus is composed of chair, secretary, and specialists in different areas (drug management, monitoring and evaluation, laboratory, radiology, surgery, and TB clinical management). Other specialists are sometimes invited (e.g. a neurologist for cases of central nervous system TB). All MDR-TB cases are reviewed by the Consilium before treatment initiation and, then, on a quarterly basis.
Results achievedSince its establishment in 2010, the Central and peripheral MDR-TB Consilia has supported the management of over 15,000 MDR-TB cases in Belarus, contributing to improvement of the diseases management throughout the country (as reported during Green Light Committee country visits in 2011, 2013 and 2017).
According to the national cohort analysis, the MDR-TB treatment success rate in Belarus increased from 37.2% in 2010 to 54.0% in 2016. The Central Consilium was pivotal in designing both new- and repurposed drugs-containing regimens in the country. Currently more than 500 M/XDR-TB patients are being treated with new and repurposed drugs. All TB specialists in the country (at least 100 physicians) were trained during Central TB Consilium sessions while presenting cases, or receiving feedback on their management.
The TB Consilium in BelgiumHistory, aims and focusIn Belgium, a low TB incidence country, the occurrence of MDR-TB and particularly XDR-TB presents a considerable challenge. The clinical experience of managing MDR-TB is concentrated among a limited number of treating physicians/specialists. In 2011, this expertise was brought together in an MDR Expert Group in close collaboration with the Inter-University Scientific Tuberculosis Committee, the Belgian Lung and Tuberculosis Association (BELTA) and the two non-profit care associations in charge of lung health and TB in Belgium: Fonds des Affections respiratoires (FARES) and Vlaamse Vereniging voor Respiratoire Gezondheidszorg en Tuberculosebestrijding (VRGT). This Committee acts as a TB Consilium with the aim of improving the management of MDR-TB cases, updating national diagnosis and treatment guidelines and collecting data for quality analysis.
Management and fundingThe TB Consilium is technically managed by BELTA-TBnet. This is a publicly funded project of BELTA covering all costs related to the diagnosis and treatment of TB that are not refunded by the health insurance (e.g. most of second-line drugs). BELTA-TBnet also promotes all useful activities needed to improve MDR-TB management and has a budget for scientific support, which covers the functioning of the TB Consilium.
Technical functioning and structureThe TB Consilium is composed of infectious disease specialists, pulmonologists, paediatricians, microbiologists, pharmacologists and public health experts. Its core function is clinical. As BELTA-TBnet is informed of any MDR-TB case treated in Belgium, the TB Consilium checks if treatment guidelines are followed and provides clinical advice as needed. Individual clinicians can contact members of the TB Consilium by e-mail, either directly or through BELTA. Clinical questions are usually answered within 2–3 working days and the BELTA coordinator transmits precise instructions to the requesting physician. The TB Consilium also approves the use of the new drugs such as bedaquiline and delamanid for individual cases. By this mechanism, it contributes to preventing the emergence of further drug resistance.
Together with BELTA-TBnet, which collects all data related to MDR-TB cases, the TB Consilium also monitors and evaluates the quality of TB-related clinical practices in Belgium. The group meets 3–4 times a year and communicates actively between meetings to share new scientific information, discuss individual cases and revise existing recommendations. Some members of the Belgian TB Consilium are also experts for the ERS/WHO electronic TB Consilium.
Results achievedMost of the MDR-TB cases treated in Belgium since 2011 have benefited from the advice of the TB Consilium. Core clinical questions concerned treatment regimen and duration. The prescription of bedaquiline was strictly monitored. From 2011 to 2016, a total of 92 MDR-TB cases were diagnosed, including 5 children. There were 24 pre-XDR (1 child) and 10 XDR-TB cases. Five of the patients were never put on treatment and 9 are still being treated. Of the remaining 78 cases, 72 were cured or completed therapy, which means Belgium achieved a treatment success rate of 92.3%. Of the remaining patients 5 were transferred out and 1 died. This high treatment success rate (reaching 100% for the 10 XDR-TB patients) reflects the efficacy of the Belgian TB Consilium.
The Belgian model of MDR-TB management was recognized as an example of best practices by the WHO in 2013.21
The TB Consilium in FranceHistory, aims and focusBased on a retrospective study showing poor treatment outcomes of MDR-TB in France22 the French National Reference Centre for Mycobacteria (NRC) decided to provide assistance for MDR-TB management, including complete drug susceptibility testing and treatment advice. These treatment recommendations were initially provided by a pulmonary physician. However, the complexity of cases soon required the help of a pool of specialists. As a consequence, the French TB Consilium was launched in 2005. The aim of the Consilium is to provide treatment advice for difficult-to-treat mycobacterial infections. Most of these cases are MDR- and XDR-TB; however, drug susceptible cases are also discussed, as well as non-tuberculous mycobacterial infections. In addition, the TB Consilium is committed to promoting consensus recommendations among its members in order to answer clinical questions for which no precise answer exists in the literature. Among these, specific recommendations have been provided for anti-tuberculosis drugs therapeutic drug monitoring, duration of treatment, choice of drug combinations and, more recently, on the indications for the shortened regimen for MDR TB.
Management and fundingThe Consilium is managed and hosted by the NRC in Paris, France. The NRC is supported by an annual grant from Santé Publique France; however, no specific funding is provided currently for the Consilium.
Technical functioning and structureThe TB Consilium is composed of a multidisciplinary team including pulmonologists, infectious diseases physicians, microbiologists, paediatricians, pharmacologists, molecular epidemiologists, and other specialists. Cases are presented monthly by the treating physicians, in person or remotely, by means of a standardized case report form. It is requested that the physician in charge of the patient comes to the meeting, or calls in during the discussion, so that the team can ensure personal interaction. The final recommendation is provided to the physician in charge of the patient at the end of the discussion, orally first and then based on a written report form.
Recommendations are based on national and WHO recommendations, in addition to the clinical assessment (judgement) done by the members of the Consilium. Decisions are taken by consensus. Moreover, the French TB Consilium advice is officially required by the French Medicine Agency (ANSM) to approve the use of new drugs under compassionate use programme, and for their use beyond the standard duration (24 weeks).
Results achievedInterim reports of the activity of the TB Consilium have already been presented in different international conferences and events23 and an extensive analysis of its activity is ongoing and it will be published elsewhere.
As of today, the TB Consilium has provided treatment advice for 786 cases, since 2005, approximately half of the total MDR-TB patients reported to the NRC during the same period. Treatment advice for 47 contacts of MDR-TB cases was also given: these cases are particularly challenging, as no clear recommendations for their management are available in international guidelines. In addition, it has been recently shown that latent tuberculosis infection of contacts of MDR-TB patients can be also due to a drug susceptible TB strain.24
The TB Consilium advice has been particularly active in the introduction of new anti-tuberculosis drugs in the treatment of MDR/XDR-TB in France, promoting the access to bedaquiline and delamanid through a compassionate use/expanded access programme and supporting the (improperly-called) “off-label” use when needed. In particular, the Consilium has pioneered the use of bedaquiline beyond 6 months, performing one of the first analyses of the emergence of bedaquiline resistance under treatment.25,26
The TB Consilium in MexicoHistory, aims and focusIn 1999, the National TB Programme in Mexico recognized drug-resistant TB as a problem that required immediate attention; however, it was only between 2009 and 2010 that the programme developed the National Strategy for Health Care of Drug Resistance TB patients in Mexico. Second-line drugs have been available for the whole country since 2010; before this date the Green Light Committee (GLC) approved their use only for 3 states: Tamaulipas, Nayarit and Veracruz. Between 2009–2010 and 2011–2013, the TB drug-resistant programme was technically supported by an International Union Against Tuberculosis and Lung Diseases (IUATLD) advisor, through a Programme for Appropriate Technology in Health (PATH) project. This contributed to implementing and then strengthening the national drug-resistant TB strategy in Mexico.
The National TB Programme developed a support network for the diagnosis and treatment of drug resistant TB cases in each state of the Mexican Republic; at present the network (which is called COEFAR – Comité Estatal de farmacoresistencia) includes 32 supporting groups in different states.
The main aims of COEFAR are the following:
- 1
To ensure that drug-resistant TB cases are properly diagnosed, treated and followed-up based on the National TB guidelines, which were published in 2010.27
- 2
To discuss the TB cases harbouring drug resistant strains of M. tuberculosis and ensure their correct management.
In order to fulfil its mission, a specific TB Consilium has been implemented within COEFAR.
Management and fundingThe Mexican TB Programme is, essentially, funded through general taxation. TB diagnosis and treatment are available free of charge in the whole country.
Technical functioning and structureThe Mexican TB Consilium (called GANAFAR, Grupo Asesor Nacional en Farmacoresistencia) is composed of the following experts: the NTP director and coordinators; the national clinical leader in drug-resistant TB; the InDRE (Instituto nacional de Referencia Epidemiológica) mycobacterial laboratory manager; some physicians belonging to the different health institutions in Mexico (with experience in managing drug-resistant TB), and a bioethics representative of the National Human Rights Commission.
In the early stages of the TB Consilium implementation, its members used to meet once every two months (or only when necessary), in face-to-face meetings where clinical cases were discussed either in person or via teleconference. More recently, in order to accelerate TB patient care, most of the cases are reviewed by e-mail, and only some very-difficult-to-treat cases are discussed during webex meetings.
The GANAFAR functions are mainly aimed at: (1) advising the COEFAR on any issue related to drug-resistant TB; (2) reviewing, recommending and ratifying documents previously approved by COEFAR; (3) updating the national TB Guidelines; (4) supporting the national TB programme in training staff on drug-resistant TB management. Since all difficult-to-treat TB cases are reviewed by the GANFAR, recently, the TB Consilium has also operated as a gateway to access treatment with the new drugs (delamanid and bedaquiline).
Results achievedBetween 2010 and August 2017, 240 cases (approximately 30 per year, e.g. 12% of the national burden of drug-resistant cases) have been discussed within the TB Consilium, including 20 XDR, 70 pre-XDR cases (MDR-TB with additional resistance to either a fluoroquinolone or an injectable drug) and 44 paediatric cases (≤17 years of age).
Between 2010 and 2017, 1785 drug-resistant cases have been diagnosed in Mexico, of whom 90% started treatment with second-line drugs; all the cases were evaluated by the Local Committee under the supervision of the National TB Programme and of the TB Consilium (when requested).
The treatment outcomes achieved in Mexico between 2010 and 2014 are as follows: treatment success 70%, lost to follow-up 14%, failure 5% and death 11%. The National Programme is committed to reducing the proportion of patients lost to follow-up and the death rate.
Recently the Mexican TB Consilium (in collaboration with the ERS/WHO TB Consilium) was able to initiate treatment with new drugs (bedaquiline and/or delamanid) though compassionate use programmes in 2 patients.
The TB Consilium in PortugalHistory, aims and focusThe Portuguese National Health Service (NHS) includes all services and entities (public and private) providing health care (primary care centres, hospitals and local health units) and aims to ensure universal health coverage of the population. The National Tuberculosis Programme (NTP) is part of the National Health Service, with a national coordination team with seven regional coordinators, responsible for defining guidelines and regulation, and coordinating TB activities and planning strategies.
In 2007, the National TB Programme defined the specific strategies necessary to control MDR-TB, based on the WHO Global Plan to Stop TB (2006–2015) and the National Reference Centre for M/XDR-TB was created in June 2007. Needing to decentralize the approach of M/XDR TB cases in a regional structure, the Health National Directorate proposed the creation of 7 Regional Reference Centres for MDR-TB (RRC), one for each of the 7 Health Regions of the country.
Management and fundingThe Portuguese NTP is essentially funded through general taxation. TB diagnosis and treatment are delivered through NHS free of charge.
Technical functioning and structureThe TB programme is centred on Primary Health Care with TB out-patient centres. These TB out-patient centres are responsible for diagnosis, treatment of TB cases and screening of groups at risk. Hospitalization is only considered in severe cases and limited to the time needed to stabilize the patient and optimize his/her treatment.
The RRC are responsible for the clinical management of all MDR-TB cases including the design (and, if necessary the modification) of the treatment regimen, the management of the adverse effects; they also decide if hospitalization is needed.
They report to the National Reference Centre, being responsible for surveillance and case analysis, while defining strategies and providing advice for difficult-to-treat cases.
The Northern Regional Reference Centre started its activity in 2009 (the first in the country), while the Lisbon Regional Reference Centre was the last, in 2013. So, only after 2013 did Portugal develop a uniform national procedure for the clinical management of MDR-TB cases.
RRC are notified on the existence of an MDRTB case by different channels: by mail (when the clinician asks for help), but also by means of two surveillance systems (the ‘specific’ TB surveillance system and general public health one) or by the Regional Pharmacy where all second-line drugs are centralized. The clinicians and the laboratory staff, in fact, need to activate these two last surveillance platforms.
Mycobacteriology evaluation and drug susceptible tests are performed by the national reference laboratory in Lisbon. Medication is provided by a centralized regional pharmacy free of charge and delivered wherever the patient is managed (outpatient centre or hospital unit). After hospital discharge, the regional reference centre provides periodic appointments for the patients with the aim of assessing disease progression and occurrence of adverse events. Together with the family physician and the public health authority, the RRC also identifies the best strategy for contact tracing.
Results achievedBased on 2013 and 2014 national cohort analysis, the RRC provided assistance to 77 of the 81 MDRTB patients diagnosed in the country – in two cases the diagnosis was post-mortem and two patients left the country before initiating treatment. The prevalence of XDR-TB was as high as 23%. The success rate was 71.6%.
The TB Consilium in United KingdomHistory, aims and focusSince 2000, there have been approximately 50 cases of MDRTB a year In the UK.28 Consultations with the Joint Tuberculosis Committee (JTC), the ethics committee of the British Medical Association, the Medical Defence Union and the Medical Protection Society prepared the ground for a web-based advisory service in 2007 – the MDR-TB Advisory Service. The service was taken over by Public Health England (PHE) and co-ordinated by the British Thoracic Society (BTS) from July 2011, being renamed the BTS MDRTB Clinical Advisory Service. The platform is currently undergoing a further revision to include outcome data and is due to be launched 1 October 2017.
Management and fundingStart-up funding was obtained from Genus Pharma, similar to Otsuka's funding of the ERS Consilium.29 From 2011, funding was obtained from the UK government (PHE). The BTS acts via a dedicated administrator and managerially through the UK JTC. Thirty-five experts were drafted in from the BTS, British Infection Society and from the Health Protection Agencies. They gave their advice free of charge and performed this task as a service, without compensation by the National Health Service (NHS). All advisors are required to complete an annual conflict of interest declaration by the BTS.
Technical functioning and structureThe website was designed to be secure, with access to designated experts. Those seeking advice could only access the responses regarding their own patients. All patient data and the referring clinician were anonymous, but advisors were identified by name.
Cases were identified as MDR-TB by the Mycobacteria Reference Laboratories and invited to seek advice as to management. Referring clinicians provided clinical data: age, sex, country of birth, whether there was known contact with a case of MDRTB, site of disease, sputum smear status, a description of the current episode, followed by the resistance pattern according to the WHO groups.
Advisors are notified by email of the request. Responses are usually made within 24h, but occasionally a longer delay results in an additional email from the co-ordinator. Advisors are able to see all comments made on the case. To date there has been no summary, so that the referring clinician can assess the responses and maintain clinical responsibility by choosing which advice to take. However, from 1 October 2017, a more formal approach to summarizing advice is intended and the panels involved will have their time funded by the NHS.
The advisory panel were invited to meet every 6 months to discuss the running of the service and any suggestions for improvement. The new service is intended to have a smaller panel to manage these aspects as well as summarize advice.
Results achievedAdvice has been given on 385 cases (18 paediatric cases) since July 2011. As previously reported for the years 2008 and 2009,29 just over half of all MDR-TB notified within the UK have been discussed in the forum and this proportion has remained constant. From review of the discussion, the vast majority had difficulty designing a drug regimen despite following the WHO guidance.30,31 The problems relate to adverse effects of drugs and decisions regarding suitable alternatives, complex co-morbidities and the need for approval by the service before bedaquiline and delamanid can be funded. There have been >22 cases of XDR-TB (data for January 2010–June 2011 not included) that have all received advice.
In addition, there have been discussions regarding rifampicin mono-resistance, preventive treatment for contacts of MDR-TB, difficult non-tuberculous mycobacteria and the management of isoniazid mono-resistance, indicating that these areas are also problematic for practising physicians.
In the last two years, interpretation of molecular resistance data has been required. Discrepancies between molecular resistance and drug susceptibility testing have occasioned frequent comment.
Advice uses current literature as an evidence-base from which to extrapolate opinions. Clinician feedback has been uniformly good (29, and unpublished data).
ConclusionsThe present survey enables a comparative analysis on how TB Consilia operating in the different countries work, based on the country-specific needs and legal regulations in force.
Although the overall aim is similar in all countries (improve diagnosis and clinical management of M/XDR-TB cases while preventing the selection of resistant mutants) significant differences exist among the different national Consilia.
In particular, not all of them are designed to record data electronically with a view to possible further analysis on how the guidelines in force are applied) and to record treatment outcomes. Moreover important differences exist in how the process is managed, with different levels of decentralization (reflecting the prevalence of the diseases and the size of the country) and different operational procedures.
The results of the survey demonstrate that the implementation of TB Consilia was useful in improving the clinical management of M/XDR-TB in the countries investigated and that room for further collaboration among the different Consilia exists.
Funding sourceThis research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Conflicts of interestThe authors have no conflicts of interest to declare.
The paper is part of the ERS/ALAT and the ERS/SBPT collaborative projects (ERS: European Respiratory Society; ALAT: Latino-American Society of Respiratory Medicine; SBPT: Brazilian Society of Pulmonology).