Enlargement of the bronchial arteries with bleeding, is more prominent in bronchial disease (bronchiectasis or chronic bronchial inflammation), than in chronic parenchymal lung disease.1
Normal bronchial arteries are small vessels (less than 2mm) that arise directly from the descending thoracic aorta. There are anatomical variations, but the most constant vessel is the right intercostobronchial trunk, which usually arises from the right posterolateral aspect of the thoracic aorta.2
Bronchial artery aneurysm (BAA) is very rare and is reported in less than 1% of selective bronchial arterial angiograms.3
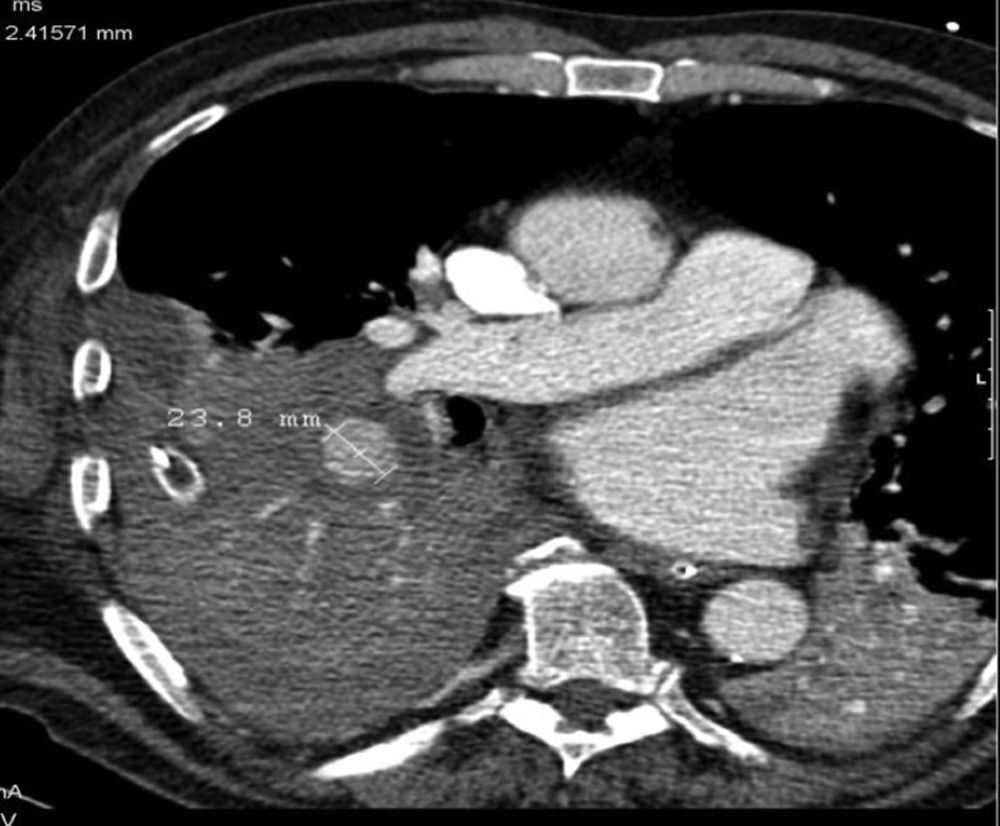
We briefly review the literature of BAA based on radiological findings of an exceptional case of an 74 years-old male, with no previous trauma or lung disease, that was admitted to our emergency department with hemoptysis and was found to have ruptured BAA in computed tomography (CT). The chest angio-CT (CT performed with intravenous contrast) revealed a 2.4cm BAA (Fig. 1) contiguous with a large right bronchial artery, that is originated from the dilated right intercostobronchial trunk, associated intrapulmonary hematoma of the lower right lobe (secondary to sustained ruptured intrapulmonary BAA) and homolateral hemothorax.
No apparent lung parenchymal or bronchial disease (namely bronchiectasis) was seen.
Thoracotomy with partial inferior right lobectomy was performed, because of the life threatening contained BAA rupture, and confirmed CT findings.
BAA can be congenital (as in the context of pulmonary sequestration or pulmonary agenesis), or can be acquired (as a result of lung disease, trauma, sepsis, vasculitis or Osler–Weber–Rendu syndrome).4 In patients without predisposing pulmonary or systemic disease, BAA are extremely rare.5
BAA are classified anatomically either as mediastinal or intrapulmonary or both, because of their associated symptoms.3 Intrapulmonary aneurysms often present hemoptysis and the main complaint for mediastinal BAA is related to compression or rupture into contiguous structures.4
Most BAA are asymptomatic until they rupture.3,4
Regardless of whether the patient has symptoms, BAA should be treated promptly when diagnosed, because it is a potentially life-threatening lesion.
Angio-CT is mandatory to make definitive diagnosis of BAA, providing essential information for further treatment approach.2,4
Thoracotomy with surgical extirpation of the aneurysm is one of the approaches, as it is embolization, for treatment of BAA and is indicated in complicated (rupture) BAA cases.4
Our case reports a complication of intrapulmonary BAA and was consistent with the extremely rare reports of BAA in patients without lung disease.